Frequently Asked Questions
General Topics
A pediatric dentist has an extra two to three years of specialized training after dental school, and is dedicated to the oral health of children from infancy through their teenage years. Children, pre-teens, and teenagers all need different approaches to deal with their behavior, guide their dental growth and development, and help them avoid future dental problems. A pediatric dentist is best qualified to meet children’s needs of all ages.
It is very important to maintain primary teeth health. Neglected cavities frequently lead to problems which affect developing permanent teeth. Primary teeth – or baby teeth – are important for (1) proper chewing and eating, (2) providing space for permanent teeth and guiding them into the correct position, and (3) permitting normal development of jaw bones and muscles. Primary teeth also affect the development of speech and add to an attractive appearance. While the front 4 teeth last until 6-7 years of age, the back cuspids and molars aren’t replaced with permanent teeth until age 10-13.
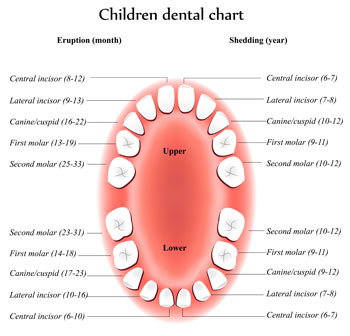 Children’s teeth begin forming before birth. As early as 4 months, the first baby teeth to erupt are the lower central incisors, followed closely by the upper central incisors. Although all 20 primary teeth usually appear by age 3, the pace and order of their eruption varies.
Children’s teeth begin forming before birth. As early as 4 months, the first baby teeth to erupt are the lower central incisors, followed closely by the upper central incisors. Although all 20 primary teeth usually appear by age 3, the pace and order of their eruption varies.
Permanent teeth begin appearing around age 6, starting with the first molars and lower central incisors. At age 8, you can generally expect the bottom 4 primary teeth (the lower central and lateral incisors) and the top 4 primary teeth (the upper central and lateral incisors) to be gone and permanent teeth to have taken their place. There is a one to two year break from ages 8-10, and then the rest of the permanent teeth will start to come in. This process continues until approximately age 21.
Adults have 28 permanent teeth, or up to 32 including the third molars (called wisdom teeth).
 Toothache:
Toothache:
Clean the area of the affected tooth thoroughly. Rinse your mouth vigorously with warm water, or use dental floss to dislodge impacted food or debris. DO NOT place aspirin on the gum or on the aching tooth. If your face is swollen, apply a cold compression and contact your dentist immediately.
Cut Tongue, Lip or Cheek: Apply ice to the affected area(s). If there is bleeding, apply firm but gentle pressure with a gauze or cloth. If the bleeding cannot be controlled by simple pressure, call a doctor or visit the emergency room.
Knocked Out Permanent Tooth: If possible, find the tooth. Handle the tooth by
the crown, and be careful not to touch the root portion. You may rinse the tooth but DO NOT clean or handle the tooth excessively. Inspect the tooth for fractures. If it is sound, try to reinsert it in its socket. Hold the tooth in place by gently biting on a gauze or clean cloth. If you cannot reinsert the tooth, place the tooth in a cup containing the saliva of the person that lost it, or use milk, but NOT water. The tooth may also be carried in the mouth beside the cheek. The person who lost their tooth must see a dentist IMMEDIATELY! Time is a critical factor in saving the tooth.
Knocked Out Baby Tooth: Contact your pediatric dentist. Unlike a permanent tooth, the baby tooth should not be replanted due to possible damage to the developing permanent tooth. In most cases, no treatment is necessary.
Chipped/Fractured Permanent Tooth: Time is a critical factor, contact your pediatric dentist immediately to reduce the chance of infection or the need for extensive dental treatment. Rinse the mouth with water and apply a cold compress to reduce swelling. If you can find the broken tooth piece, bring it with you to the dentist in a glass of milk, or the person’s saliva. DO NOT USE WATER TO TRANSPORT A CHIPPED TOOTH.
Chipped/Fractured Baby Tooth: Contact your pediatric dentist.
Severe Blow to the Head: Call 911 immediately or take your child to the nearest emergency room.
Possible Broken or Fractured Jaw: Keep the jaw from moving and take your child to the nearest emergency room.
Read more about how to prevent dental emergencies during recreational activities and sports with mouth guards.
Radiographs (X-Rays) are a vital and necessary part of your child’s dental diagnostic process. Without them, certain dental conditions can be missed.
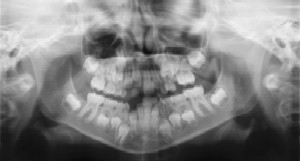
Radiographs allow dentists to diagnose and treat health conditions that cannot be detected during a clinical examination, and they detect much more than cavities. For example, radiographs may be needed to survey erupting teeth, diagnose bone diseases, evaluate the results of an injury, or plan orthodontic treatment. If dental problems are found and treated early, dental care is more comfortable for your child and more affordable for you.
The American Academy of Pediatric Dentistry recommends radiographs and examinations every six months for children with a high risk of tooth decay. On average, most pediatric dentists request radiographs approximately once a year. Approximately every 3 years, it is a good idea to obtain a complete set of radiographs, either a panoramic and bitewings or periapicals and bitewings.
Pediatric dentists are particularly careful to minimize the exposure of their patients to radiation. With contemporary safeguards, the amount of radiation received in a dental X-ray examination is extremely small. The risk is negligible. In fact, dental radiographs represent a far smaller risk than an undetected and untreated dental problem. Today’s equipment filters out unnecessary x-rays and restricts the x-ray beam to the area of interest. High-speed film and proper shielding assure that your child receives a minimal amount of radiation exposure.
 Tooth brushing is one of the most important tasks for good oral health. But, many toothpastes and tooth polishes can damage young smiles with harsh abrasives, which can wear away young tooth enamel. When looking for a toothpaste for your child, make sure to pick one that is recommended by the American Dental Association, as shown on the box and tube. These toothpastes have undergone testing to insure they are safe to use.
Tooth brushing is one of the most important tasks for good oral health. But, many toothpastes and tooth polishes can damage young smiles with harsh abrasives, which can wear away young tooth enamel. When looking for a toothpaste for your child, make sure to pick one that is recommended by the American Dental Association, as shown on the box and tube. These toothpastes have undergone testing to insure they are safe to use.
Use only a smear of toothpaste (the size of a grain of rice) to brush the teeth of a child less than 3 years of age. For children 3 to 6 years old, use a pea-sized amount of toothpaste and perform or assist your child’s toothbrushing. Remember that young children do not have the ability to brush their teeth effectively on their own. Children should not swallow excess toothpaste after brushing
Parents are often concerned about their children grinding their treeth while they sleep (bruxism). Often, the first indication of bruxism is the noise created by the grinding, or, the parent may notice teeth wearing down. One theory is that psychology affects bruxism. Stress due to a new environment, divorce, changes at school, etc. can influence a child to grind their teeth. Another theory links pressure in the inner ear. If there are pressure changes (like in an airplane during take-off and landing, when people are chewing gum, etc.) the child will grind by moving their jaw to relieve this pressure.
The majority of cases of pediatric bruxism do not require any treatment. If excessive wear of the teeth – attrition – is present, then a nightly mouth guard may be prescribed. The good news is that most children outgrow bruxism. The grinding typically decreases between the ages of 6-9 and children tend to stop grinding altogether between ages 9-12. If you suspect bruxism, discuss this with your pediatrician or pediatric dentist.
 Sucking is a natural reflex in infants and young children. They may use thumbs, fingers, pacifiers and other objects on which to suck. It makes them feel secure and happy, or provides a sense of security during difficult periods. Since thumb sucking is relaxing, it may induce sleep.
Sucking is a natural reflex in infants and young children. They may use thumbs, fingers, pacifiers and other objects on which to suck. It makes them feel secure and happy, or provides a sense of security during difficult periods. Since thumb sucking is relaxing, it may induce sleep.
Thumb sucking that persists beyond the eruption of the permanent teeth can cause problems with the proper growth of the mouth and tooth alignment, and the intensity at which a child sucks on fingers or thumbs will determine whether or not dental problems may result. Children who rest their thumbs passively in their mouths are less likely to have difficulty than those who vigorously suck their thumbs.
Children should cease thumb sucking by the time their permanent front teeth are ready to erupt. Usually, children stop between the ages of 2 and 4. Peer pressure causes many school-aged children to stop.
Pacifiers are no substitute for thumb sucking. They can affect the teeth essentially the same way as sucking thumbs. However, pacifier use can be controlled and modified more easily than the thumb or finger habit. Consult your pediatric dentist if you have concerns about thumb sucking or pacifier use.
A few suggestions to help your child quit thumb sucking:
- Children often suck their thumbs when feeling insecure. Focus on correcting the cause of anxiety, instead of the thumb sucking.
- Children who are sucking for comfort will feel less inclined to indulge the habit when their parents provide comfort.
- Reward children when they refrain from sucking during difficult periods, such as when being separated from their parents.
- Your pediatric dentist can encourage your child to stop sucking and explain what could happen if they continue.
- If these approaches don’t work, remind your child of their habit by bandaging the thumb or putting a sock on their hand at night. Your pediatric dentist may recommend the use of a mouth appliance.
Inside the tooth, under the enamel and a hard layer called the dentin, is a soft tissue called pulp. The pulp contains blood vessels, nerves, and connective tissue and creates the hard tissues surrounding the tooth during development. The pulp extends from the crown of the tooth to the tip of the roots – where it connects to the tissues surrounding the root. The pulp is important during a tooth’s growth and development The purpose of pulp therapy in Pediatric Dentistry is to maintain the vitality of the affected tooth so that the tooth is not lost.
Dental caries (cavities) and traumatic injury are the main reasons for a tooth to require pulp therapy. Pulp therapy is often referred to as a “nerve treatment”, “children’s root canal”, “pulpectomy” or “pulpotomy”. The two common forms of pulp therapy in children’s teeth are the pulpotomy and pulpectomy.
A pulpotomy removes the diseased pulp tissue within the crown portion of the tooth. Next, an agent is placed to prevent bacterial growth and to calm the remaining nerve tissue. This is followed by a final restoration, which is usually a stainless steel crown.
A pulpectomy is required when the entire pulp is affected into the root canal of the tooth. During this treatment, the diseased pulp tissue is completely removed from both the crown and root. The canals are cleansed, disinfected and, in the case of primary teeth, filled with a resorbable material. Then, a final restoration is placed. A pulpectomy for a permanent tooth would be filled with a non-resorbing material.
 Developing malocclusions – or bad bites – can be recognized as early as 2-3 years of age. Often, early steps can be taken to reduce the need for major
Developing malocclusions – or bad bites – can be recognized as early as 2-3 years of age. Often, early steps can be taken to reduce the need for major
orthodontic treatment at a later age.
Stage I – Early Treatment: This period of treatment encompasses ages 2 to 6. At this young age, we are concerned with underdeveloped dental arches, the premature loss of primary teeth, and harmful habits such as finger or thumb sucking. Treatment initiated during this stage of development is often very successful and many times, though not always, can eliminate the need for future orthodontic/orthopedic treatment.
Stage II – Mixed Dentition: This period covers the ages of 6 to 12, with the eruption of the permanent incisor (front) teeth and 6 year molars. Treatment concerns deal with jaw malrelationships and dental realignment problems. This is an excellent stage to start treatment, when indicated, as your child’s hard and soft tissues are usually very responsive to orthodontic or orthopedic forces.
Stage III – Adolescent Dentition: This stage deals with the permanent teeth and the development of the final bite relationship.
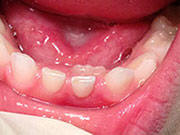 This is a very common occurrence with children, and is usually the result of a lower baby tooth not falling out when the permanent tooth is erupting. In most cases, it will usually fall out on its own within two months. If it doesn’t, then contact your pediatric dentist because they can easily remove the tooth. The permanent tooth should then slide into its proper place.
This is a very common occurrence with children, and is usually the result of a lower baby tooth not falling out when the permanent tooth is erupting. In most cases, it will usually fall out on its own within two months. If it doesn’t, then contact your pediatric dentist because they can easily remove the tooth. The permanent tooth should then slide into its proper place.
Early Infant Oral Care
 The American Academy of Pediatric Dentistry (AAPD) recommends that all pregnant women receive oral healthcare and counseling during pregnancy. Research has shown evidence that periodontal disease can increase the risk of preterm birth and low birth weight. Talk to your doctor or dentist about ways you can prevent periodontal disease during pregnancy.
The American Academy of Pediatric Dentistry (AAPD) recommends that all pregnant women receive oral healthcare and counseling during pregnancy. Research has shown evidence that periodontal disease can increase the risk of preterm birth and low birth weight. Talk to your doctor or dentist about ways you can prevent periodontal disease during pregnancy.
Additionally, mothers with poor oral health may be at a greater risk of passing cavity-causing bacteria to their young children. Mother’s should follow these simple steps to decrease the risk of spreading the bacteria:
- Visit your dentist regularly.
- Brush and floss on a daily basis to reduce bacterial plaque.
- Maintain a proper diet, and reduce beverages and foods high in sugar & starch.
- Use a fluoridated toothpaste recommended by the ADA and rinse every night with an alocohol-free, over-the-counter mouth rinse with .05 % sodium fluoride in order to reduce plaque levels.
- Don’t share utensils, cups or food which can transmit cavity-causing bacteria to your children.
- Using xylitol chewing gum – 4 pieces per day by the mother – can decrease a child’s odds of cavities.
The American Academy of Pediatrics (AAP), the American Dental Association (ADA), and the American Academy of Pediatric Dentistry (AAPD) all recommend establishing a “Dental Home” for your child by their first birthday. Children who have a dental home are more likely to receive appropriate preventive and routine oral health care.
The Dental Home is intended to provide a place for dental care other than the Emergency Room.
You can make their first visit enjoyable and positive. If old enough, your child should be informed of the visit and told that the dentist and their staff will explain all procedures and answer any questions. The less to-do concerning the visit, the better.
It is best if you refrain from using words around your child that might cause unnecessary fear, such as needle, pull, drill or hurt. Pediatric dental offices make a practice of using words that convey the same message, but are pleasant and non-frightening to the child.
Teething is the process of baby teeth coming through the gums into the mouth. It is variable among individual babies; some babies get their teeth early and some get them late. In general, the first baby teeth to appear are usually the lower front (anterior) teeth and they usually begin erupting between the age of 6-8 months. See
“Eruption of Your Child’s Teeth” for more details.
 One serious form of decay among young children is baby bottle tooth decay. This condition is caused by frequent and long exposures of an infant’s teeth to liquids that contain sugar. Among these liquids are milk (including breast milk), formula, fruit juice and other sweetened drinks.
One serious form of decay among young children is baby bottle tooth decay. This condition is caused by frequent and long exposures of an infant’s teeth to liquids that contain sugar. Among these liquids are milk (including breast milk), formula, fruit juice and other sweetened drinks.
Putting a baby away for a nap, or to bed at night with a bottle containing liquids other than water can cause serious and rapid tooth decay. Sweet liquid pools around the child’s teeth giving plaque bacteria an opportunity to produce acids that attack tooth enamel. If you must give the baby a bottle as a comforter at bedtime, it should contain only water. If your child won’t fall asleep without the bottle and its usual beverage, gradually dilute the bottle’s contents with water over a period of two to three weeks.
After each feeding, wipe the baby’s gums and teeth with a damp washcloth or gauze pad to remove plaque. The easiest way to do this is to sit down and place the child’s head in your lap. Or, you can lay the child on a dressing table or the floor. Whatever position you use, be sure you can see into the child’s mouth easily.
Sippy cups should be used as a training tool to transition your child from the bottle to a cup. If your child uses a sippy cup throughout the day, fill the sippy cup with water only, except at mealtimes when you can use other sugar free beverages in moderation. By filling the sippy cup with liquids that contain sugar like milk, fruit juice, sports drinks, etc., and allowing a child to drink from it throughout the day, it soaks the child’s teeth in cavity causing bacteria.Water should be your child’s bevevrage of choice, and what they drink most often.
Prevention
 Brushing Tips:
Brushing Tips:
- Starting at birth, clean your child’s gums with a soft cloth and water.
- As soon as your child’s teeth erupt, brush them with a soft-bristled toothbrush.
- If they are under the age of 2, use a small smear of toothpaste.
- If they’re 2-5 years old, use a pea-size amount of toothpaste.
- Be sure and use an ADA-accepted fluoride toothpaste and make sure your child does not swallow it.
- The parent should brush the child’s teeth until they are old enough to do a good job on their own.
Flossing Tips:
- Flossing removes plaque between teeth and under the gumline where a toothbrush can’t reach.
- Flossing should begin when any two teeth touch.
- Be sure and floss your child’s teeth daily until he or she can do it alone.
 Healthy eating habits lead to healthy teeth. Like the rest of the body, teeth, bones and the soft tissues of the mouth need a well-balanced diet. Children should eat a variety of foods from the five major food groups. Most pre-packaged snacks that children eat can lead to cavity formation. Thus, the more frequently a child snacks, the greater the chance for tooth decay. How long food remains in the mouth also plays a role. For example, hard candy and breath mints stay in the mouth a long time, which cause longer acid attacks on tooth enamel. If your child must snack, choose nutritious foods such as vegetables, low-fat yogurt, and low-fat cheese, which are healthier and better for children’s teeth.
Healthy eating habits lead to healthy teeth. Like the rest of the body, teeth, bones and the soft tissues of the mouth need a well-balanced diet. Children should eat a variety of foods from the five major food groups. Most pre-packaged snacks that children eat can lead to cavity formation. Thus, the more frequently a child snacks, the greater the chance for tooth decay. How long food remains in the mouth also plays a role. For example, hard candy and breath mints stay in the mouth a long time, which cause longer acid attacks on tooth enamel. If your child must snack, choose nutritious foods such as vegetables, low-fat yogurt, and low-fat cheese, which are healthier and better for children’s teeth.
The Dental Home is intended to provide a place for dental care other than the Emergency Room.
You can make their first visit enjoyable and positive. If old enough, your child should be informed of the visit and told that the dentist and their staff will explain all procedures and answer any questions. The less to-do concerning the visit, the better.
It is best if you refrain from using words around your child that might cause unnecessary fear, such as needle, pull, drill or hurt. Pediatric dental offices make a practice of using words that convey the same message, but are pleasant and non-frightening to the child.
Good oral hygiene removes bacteria and the left over food particles that combine to create cavities. For infants, use a wet gauze or clean washcloth to wipe the plaque from teeth and gums. Avoid putting your child to bed with a bottle filled with anything other than water. See “Baby Bottle Tooth Decay” for more information.
For older children, brush their teeth at least twice a day for two minutes at a time. Also, watch the number of snacks containing sugar that you give your children.
The American Academy of Pediatric Dentistry recommends visiting the dentist every six months, beginning at your child’s first birthday. Routine visits will start your child on a lifetime of good dental health.
Your pediatric dentist may also recommend protective sealants or home fluoride treatments for your child. Sealants can be applied to your child’s molars to prevent decay on hard to clean surfaces.
“Eruption of Your Child’s Teeth” for more details.
A sealant is a protective coating that is applied to the chewing surfaces of the back teeth (premolars and molars), where four out of five cavities in children are found. Sealant acts as a barrier to food, plaque and acid, thus protecting the decay-prone areas of the teeth.
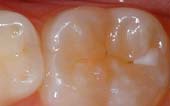
Before Sealant Applied
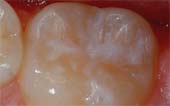
After Sealant Applied
Fluoride is a naturally occurring element which has shown to prevent tooth decay by as much as 50-70%. For children younger than 8 years old, fluoride actually helps strengthen the adult teeth that are developing beneath their gums. With little or no fluoride, teeth aren’t strengthened enough to help them resist cavities. Excessive fluoride ingestion by young children can lead to dental fluorosis, which is a white discoloration (brown in advanced cases) of the permanent teeth.
The two primary sources of fluoride are fluoridated water and toothpaste. Fluoridated water is most commonly found in local tap water. Dentists encourage drinking tap water from the sink because a number of water dispensing refrigerators filter out up to 90% of fluoride found in local water. However, charcoal and carbon type water filters such as a Britta filter retain fluoride levels found in local water while still providing filtered drinking water.
For children beneath 3 years of age, use a smear of fluoride toothpaste (the size of a grain of rice) to brush their teeth. For children 3 to 6 years old, use a “pea-size” amount of toothpaste and perform or assist your child’s tooth brushing. To ensure that your child’s toothpaste contains the optimal amount of fluoride, look for the ADA seal of acceptance somewhere on the packaging. Children should not swallow excess toothpaste after brushing, in order to avoid fluorosis. Be sure to follow your pediatric dentist’s instructions on suggested fluoride use and possible supplements.
Awareness of a child’s potential sources of fluoride can help parents prevent the possibility of dental fluorosis.
Some sources of fluoride are:
- Fluoridated toothpaste.
- Fluoride supplements.
- Tap water.
Two and three-year olds may not be able to spit out toothpaste when brushing. As a result, younger children may ingest an excessive amount of fluoride when brushing. Toothpaste ingestion during this period of permanent tooth development is the greatest risk factor for developing of fluorosis.
Excessive intake of fluoride supplements may also contribute to fluorosis. Fluoride drops and tablets, as well as fluoride fortified vitamins should not be given to infants younger than six months of age. After that time, fluoride supplements should only be given to children after all of the sources of ingested fluoride have been accounted for and upon the recommendation of your pediatrician or pediatric dentist.
Certain foods contain high levels of fluoride, especially: powdered concentrate infant formula, soy-based infant formula, infant dry cereals, creamed spinach, and infant chicken products. Please read the label or contact the manufacturer to learn more about the fluoride levels in specific foods.
Some beverages also contain high levels of fluoride, especially: decaffeinated teas, white grape juices, and juice drinks manufactured in fluoridated cities. Soft drinks served at restaurants may also contain fluoride, depending upon the fluoridation levels in their local water supply.
Parents can take the following steps to decrease the risk of fluorosis in their children’s teeth:
- Use baby teeth cleanser on a toothbrush in very young children.
- Use only a pea-sized drop of children’s toothpaste when brushing.
- Account for all of the sources of ingested fluoride before requesting fluoride supplements from your child’s physician or pediatric dentist.
- Avoid giving any fluoride supplements to infants until they are at least 6 months old.
- Obtain fluoride level test results for your drinking water before giving fluoride supplements to your child. To do this, check with local water utilities.
 Oral injuries can occur if you participate in recreational activities and organized sports. Which makes a properly fitted mouth guard – or mouth protector – an important piece of athletic gear that can help protect your smile. A mouth guard should be used during any activity that could result in a blow to the face or mouth.
Oral injuries can occur if you participate in recreational activities and organized sports. Which makes a properly fitted mouth guard – or mouth protector – an important piece of athletic gear that can help protect your smile. A mouth guard should be used during any activity that could result in a blow to the face or mouth.
Mouth guards help prevent broken teeth, injuries to the lips, tongue, face, and jaw. A properly fitted mouth guard will stay in place while you’re wearing it, making it easy for you to talk and breathe.
Ask your dentist about custom and store-bought mouth protectors.
The American Academy of Pediatric Dentistry (AAPD) recognizes the benefits of xylitol for the oral health of infants, children, adolescents, and persons with special health care needs.
Mothers chewing xylitol gum 2-4 times per day can reduce cavities up to 70% in their children aged 3 months to 5 years.
Studies using xylitol as either a sugar substitute or a small dietary addition have demonstrated a dramatic reduction in new tooth decay, and some reversal of existing dental cavities. Xylitol provides additional protection that enhances all existing prevention methods. The xylitol effect is long-lasting and possibly permanent. Low decay rates persisted years after the trials completed.
Xylitol is distributed throughout nature in small amounts. Some great sources of xylitol are fruits, berries, mushrooms, lettuce, hardwoods, and corn on the cob. One cup of raspberries contains less than one gram of xylitol.
Studies suggest that consuming 4-20 grams of xylitol per day divided into 3-7 consumption periods produces the most positive results. Greater results did not occur in larger consumption and may lead to diminishing results. Similarly, consumption frequency of less than 3 times per day showed no effect.
Visit your local health food store or search online to find products containing 100% xylitol. Consult your dentist about xylitol, and the amount you should specifically consume.
Sports drinks have erosive properties and the ability to dissolve fluoride-rich enamel that can lead to cavities. The negative effects of sports drinks are due to the dense sugar content and the high amount of acid.
Children should avoid sports drinks and hydrate with water before, during and after sports to minimize dental problems. Be sure to talk to your pediatric dentist before consuming sports drinks.
If sports drinks are consumed:
- Reduce the frequency and contact time.
- Swallow immediately and do not swish them around the mouth.
- Neutralize the effect of sports drinks by alternating sips of water with the drink.
- Rinse mouthguards only in water.
- Seek out dentally friendly sports drinks.
- Consider diluting sports drinks with 50% water.
Adolescent Dentistry

You might not be surprised anymore to see people with pierced tongues, lips or cheeks, but you might be surprised to know just how dangerous these piercings can be.
There are many risks involved with oral piercings, including chipped or cracked teeth, blood clots, blood poisoning, heart infections, brain abscess, nerve disorders, and receding gums or scar tissue. Your mouth contains millions of bacteria, and infection is a common complication of oral piercing. Your tongue could swell large enough to close off your airway!
Common symptoms after piercing include pain, swelling, infection, an increased flow of saliva and injuries to gum tissue. Difficult-to-control bleeding or nerve damage can result if a blood vessel or nerve bundle is in the path of the needle.
Follow the advice of the American Dental Association and give your mouth a break – skip the mouth jewelry.
Tobacco in any form can jeopardize your health and cause incurable damage. Smokeless tobacco, also called dip, chew or snuff, is often used by teens who believe that it is a safe alternative to smoking cigarettes. This is an unfortunate misconception. Studies show that spit tobacco may be more addictive than smoking cigarettes and may be more difficult to quit. People who use it need to understand that one can of snuff delivers as much nicotine as 60 cigarettes. In as little as three to four months, smokeless tobacco use can cause periodontal disease and produce pre-cancerous lesions called leukoplakias.
If you are a tobacco user you should watch for the following that could be early signs of oral cancer:
- A sore that won’t heal.
- White or red leathery patches on your lips, and on or under your tongue.
- Pain, tenderness or numbness in the mouth or lips.
- Difficulty chewing, swallowing, speaking or moving your jaw or tongue; or a change in the way your teeth fit together.
Because the early signs of oral cancer usually are not painful, people often ignore them. If it’s not caught in the early stages, oral cancer can require extensive, sometimes disfiguring, surgery. Even worse, it can kill.
The best advice is to avoid tobacco in any form. By doing so, you will avoid bringing cancer-causing chemicals in direct contact with your tongue, gums and cheek.
Invisalign Orthodontics
Invisalign is a type of orthodontic treatment used to straighten teeth. It utilizes clear, custom-made aligners that fit snugly over the teeth, gradually moving them into the desired position. Unlike traditional braces, Invisalign aligners are nearly invisible, making them a popular choice for those who wish to avoid the look of metal brackets. The aligners are removable, making it easier to eat and brush teeth than with braces. Invisalign treatment typically involves a series of aligners that are changed every two weeks to continue shifting the teeth into the desired position. The length of treatment varies depending on the severity of the teeth correction needed. Invisalign is a popular option for those seeking a less noticeable orthodontic treatment that is also effective.
1. Discreet: Invisalign treatment uses clear, nearly invisible aligners, making them more aesthetically appealing than traditional metal braces.
2. Comfortable: The aligners are made of smooth, flexible material that reduces irritation and discomfort often associated with traditional braces.
3. Convenient: Patients can easily remove the aligners to eat, drink, brush, and floss, making it easier to maintain oral hygiene.
4. Predictable: Invisalign uses 3D digital imaging technology to create a customized treatment plan, ensuring precise alignment and predictable results.
5. Efficient: Invisalign treatment can often be completed in a shorter period of time than traditional braces.
6. Versatile: Invisalign can effectively treat a variety of orthodontic issues, including crowded or spaced teeth, overbites, underbites, and crossbites.
7. Easy Maintenance: Unlike traditional braces, Invisalign aligners require minimal maintenance and do not require regular adjustments.
8. Improved Confidence: Unlike traditional braces, Invisalign aligners are virtually invisible, allowing patients to feel more confident about their smile during treatment.
Invisalign treatment is a perfect option for teenagers who want to straighten their teeth without the discomfort, aesthetic concerns, and hassle that comes with traditional metal braces. There are a variety of benefits for teens who choose Invisalign. First, adolescents can wear clear, removable aligners, ensuring minimal impact on their day-to-day routines. Secondly, Invisalign offers better aesthetics, allowing teens to smile confidently and pose for pictures without being conscious of their braces. The clear aligners blend with the teeth well, making them almost invisible. Invisalign doesn’t interrupt the activities of the wearer, particularly for teens involved in sports, band, or other extracurricular activities. Finally, this treatment is significantly beneficial for special occasions like prom where teens do not want their braces to draw unwanted attention. As a result, Invisalign treatment offers teens the freedom to undergo orthodontic treatment without negatively affecting their self-esteem and everyday activities.
Invisalign treatment uses clear plastic aligners to straighten teeth, while traditional metal braces use brackets and wires. Invisalign aligners are virtually invisible and removable, making them more aesthetically pleasing and easier to clean than metal braces. Invisalign allows patients to eat and drink what they want without restrictions, whereas traditional braces require avoiding certain foods that can damage the hardware. Invisalign requires fewer office visits and typically has a shorter treatment time compared to traditional braces. However, traditional braces may be more effective for correcting certain types of dental issues, such as severe overcrowding or bite problems. They are also more durable and can withstand more force than Invisalign aligners. Ultimately, the choice between Invisalign and traditional braces will depend on an individual’s specific dental needs and preferences.
An iTero scanner is a specialized piece of technology used to create digital impressions of a patient’s teeth and mouth. It utilizes advanced laser scanning technology to create a 3D model of the patient’s teeth and gums, providing a highly accurate and detailed picture of the patient’s dental structure. The iTero scanner is frequently used by dentists and orthodontists to create customized treatment plans, such as braces or clear aligners. Patients can benefit from the iTero scanner’s non-invasive and painless process, which eliminates the need for messy and uncomfortable traditional dental impressions. The scanned images are immediately available for analysis and can be shared with patients to help them visualize their treatment options. Overall, the iTero scanner is a state-of-the-art tool that helps to streamline the dental procedures, improve accuracy, and deliver superior oral healthcare.
2. Time-efficient: The iTero scanner offers a quick and efficient alternative to traditional dental molds. This leads to faster treatment and reduces the number of appointments required.
3. Comfortable for the patient: The scanner’s wand is non-invasive and painless, allowing the patient to sit comfortably throughout the scanning process.
4. Reduced risk of contamination: Since the scanner is a digital tool, there is no risk of contamination and no need for storage facilities.
5. Improved communication: The iTero scanner provides clear and detailed 3D images, which can be easily shared with other healthcare providers.
6. Enhanced patient engagement: Patients can see a visual representation of their teeth and gums through the iTero scanner’s 3D images, enabling them to engage more effectively in their treatment plan.
7. Supporting multiple applications: iTero scanner can be utilized in various dental procedures, including orthodontics, restorative dentistry, and implant placement, among others.
Do you offer routine dentistry only?
While we do offer a wide range of cosmetic dental treatments, many of our patients only come to us for routine dentistry. You may only ever need a check-up, but it’s handy to know we can you help with more.
Will I see the same dentist?
You’ll always see the same dentist. We believe it’s important for our dentists to see the same patients, so they can get to know you as an individual – not just a medical record.
Will I be able to understand what my dentist says?
Dental jargon can be overwhelming. Our dentists will explain everything in plain English, so you’ll always know what’s going on and won’t leave the practice feeling confused.
What if I can't afford private dental care?
We appreciate private health care can be expensive. If you have private medical insurance, many of our treatments will be covered by your insurer. Finance plans are available for high-value treatments such as veneers.
Can you help if I'm scared of going to the dentist?
Visiting the dentist can be a daunting experience for many. We’re here to make your visit to the dentist as comfortable as possible, so you can get the dental care you deserve. We offer dental sedation to nervous patients, so you won’t feel or remember a thing. It’s like you never went to the dentist.
Where is the practice located?
330 W 58th St
Suite 613
New York, NY 10019
If you can’t find an answer to your question on our FAQ page, then contact us. Our friendly, helpful staff will be happy to answer any questions you have about becoming a patient, a specific treatment, rearranging an appointment, and more.
